Development of COVID-19 Vaccine
- Pengarang:
Engku Nur Syafirah E. A. R.1, Mohammad A. I. Al-Hatamleh2, Chan Yean Yean1 and Rohimah Mohamud2,
- Pengarang Koresponden:
Dr Rohimah Mohamud
Department of Immunology, School of Medical Sciences, Universiti Sains Malaysia, Health Campus, 16150, Kubang Kerian, Kelantan, Malaysia
Email: rohimahm@usm.my
Abstract
A novel coronavirus, SARS-CoV-2 or COVID-19, is a pandemic disease which affecting the whole world without mercy. It is highly infectious and virulent, unfortunately, no vaccine is available for COVID-19. Immune system is a defence mechanism which can recognise pathogen and destroy it. A vaccine characteristically consists of an agent which resembles a disease-causing organism and is frequently prepared from weakened or killed forms of organism, its toxins or one particular part of surface proteins. A vaccine prevents disease by allowing the body to quickly be more responsive to attack and increasing the immune response to particular pathogen without causing disease. This review aims to provide a background of COVID-19, currently in-use vaccine platforms and early attempts on vaccine development from both Malaysia and worldwide. This review may benefit in further understanding the disease and immune intervention of potential COVID-19 vaccine in the near future.
Introduction on COVID-19
Currently, the world is suffering from an on-going pandemic of an infectious disease, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) or COVID-19, that is highly contagious and virulent. It is a novel coronavirus pneumonia which has been identified in December 2019 in Wuhan city, Hubei Province of China1. After approximately one month, there were confirmed COVID-19 cases from three countries outside China (Thailand, Japan and South Korea) have been reported, and on 11 March 2020, the WHO declared the outbreak of SARS-CoV-2 a global pandemic2. According to a situation reported by WHO, a total of 2,241,778 confirmed cases and 152,551 deaths have been reported around the world on 19 April 20203 (Figure 1).
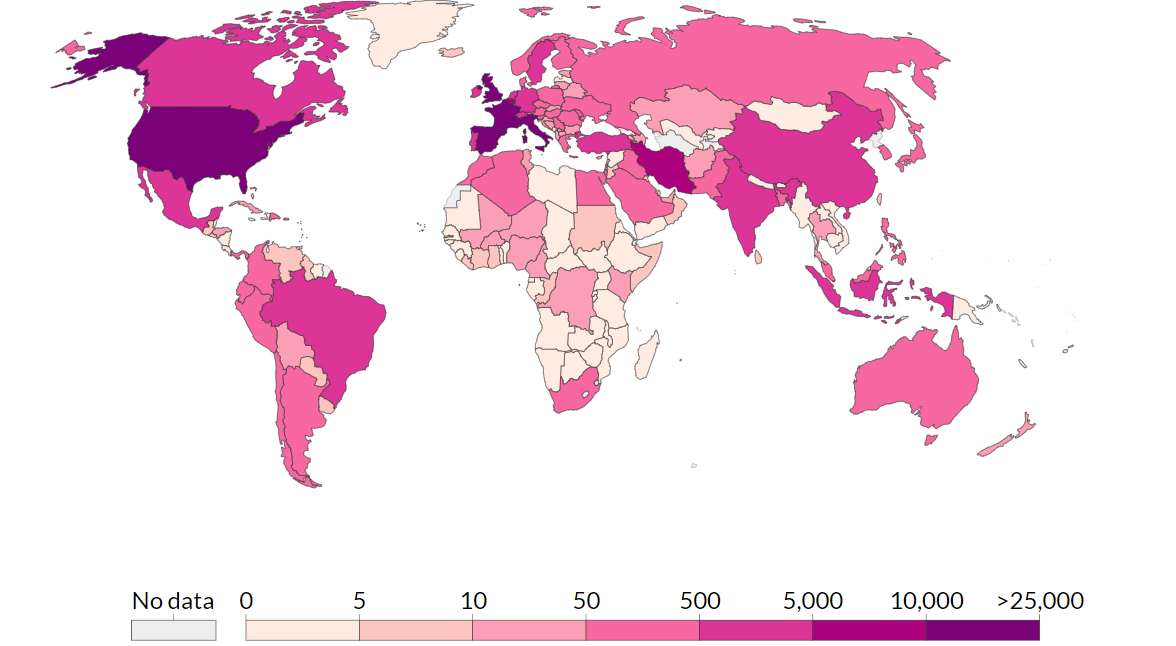
Figure 1: Distribution of the confirmed COVID-19 deaths as at 19 April 2020 4.
Various clinical manifestations were reported in patients with COVID-19 and it were ranged between mild, moderate and severe, which make this disease rapidly progressive and fulminant5. The main clinical presentations including fever, cough, and shortness of breath6,7. Additional symptoms such as loss of smell, fatigue, muscle pain, mild diarrhoea, sore throat, and abdominal pain can be seen in certain COVID-19 patients6. The incubation period of the virus can be in range of 2 - 14 days from the time of exposure to onset of symptoms8.
While majority of cases consequence in mild symptoms, but some cases progress to viral pneumonia, sepsis and multi-organ failure, subsequently leads to death. Elderly people and comorbidities patients are high risk population in getting complications from COVID-19 infection9. Interestingly, there is also a group of infected COVID-19 people that is asymptomatic but able to spread the disease to other people10. The situation urges the need to develop a vaccine against COVID-19 to control the disease spread and mortality but currently, no vaccine is available. Recently, there are several COVID-19 vaccine development projects which mostly are still in preclinical and clinical stages4. According to the largest clinical trials database (ClinicalTrials.gov), which is run by the National Institutes of Health (NIH), United States, only five projects are in the clinical stage to develop vaccine candidates for COVID-19 (Table 1).
|
Table 1: Registered clinical trials aim to develop vaccine candidates for COVID-19 (Adapted from Roser et al. 2020) |
|||||
|
Responsible Party, Country |
Vaccine |
Study Start Date |
Estimated Study Completion Date |
NCT Identifier | |
|
CanSino Biologics Inc., China |
Ad5-nCoV: Adenovirus type 5 vector that expresses S protein |
March 16, 2020 |
December 30, 2020 |
NCT04313127 |
|
|
National Institute of Allergy and Infectious Diseases (NIAID), US |
mRNA-1273: Lipid nanoparticle-encapsulated mRNA-based vaccine that encodes for a full-length, prefusion S protein of SARS-CoV-2 |
March 3, 2020 |
June 1, 2021 |
NCT04283461 |
|
|
Shenzhen Geno-Immune Medical Institute, China |
LV-SMENP-DC: Dendritic cells modified with lentiviral vector expressing synthetic mini-gene based on domains of selected viral proteins; administered with antigen-specific cytotoxic T lymphocytes |
March 24, 2020 |
December 31, 2024 |
NCT04276896 |
|
|
Inovio Pharmaceuticals, China |
INO-4800: DNA plasmid encoding S protein delivered by electroporation |
April 3, 2020 |
November 2020 |
NCT04336410 |
|
|
Shenzhen Geno-Immune Medical Institute, China |
Pathogen-specific artificial antigen-presenting cells: These cells modified with lentiviral vector expressing synthetic minigene based on domains of selected viral proteins |
February 15, 2020 |
December 31, 2024 |
NCT04299724 |
|
Introduction to vaccine
Vaccine is defined as biological agent which stimulates an immune response against a specific antigen originated from a pathogenic agent11. Earlier attempt at vaccination started in 1798 from Edward Jenner’s experiment by using cowpox to immunize against smallpox12. His revolutionary work therefore led to global eradication of smallpox in 198012. Since then, vaccines have greatly help in preventing several communicable and lethal diseases such as polio, diphtheria, pertussis, rubella, Hepatitis B, and many more.
Vaccination is classified into two forms; passive or active approaches. Passive vaccination occurs by transferring of preformed antibodies to an unvaccinated person. This person would then acquire a short-term immunity against to a particular antigen from microorganism or toxin due to the presence of these preformed antibodies. However, once these preformed antibodies are depleted, the person is no longer have immunity against this microorganism or toxin13. For instance, maternal antibodies transferred to the foetus via placenta during pregnancy is one of natural passive vaccination14. Concurrent with these results of short-term immunity, the person’s own body is feasible to be in the early stage of developing its own active immune response.
Active vaccination occurs with exposure of pathogenic agent to an unvaccinated person. Once exposed, the immune system begins to develop immunity against this agent. In contrast with passive vaccination, active vaccination produces long-lasting immunity due to activation of the individual’s immune system which has memory against the agent15. For example, exposure to one particular influenza virus is one of natural active vaccination which gives long-term immunity to the influenza virus. Stimulation of person’s immunity by vaccines are an example of artificial active vaccination. The current types of vaccine used are viable/ attenuated vaccines, inactivated vaccines, recombinant vaccines, and toxoid vaccines16. (Table 2).
Table 2: Advantages and disadvantages of different vaccine platforms
|
Vaccine types |
Advantages |
Disadvantages |
Examples |
|
Viable /Attenuated |
|
|
Viral vaccines
Bacterial vaccine
|
|
Killed/ Inactivated |
|
|
Viral vaccine
Bacterial vaccine
|
|
Recombinant protein |
|
|
Viral vaccine
Bacterial vaccine
|
|
Toxoid |
|
|
Bacterial vaccine
|
Herd immunity from COVID-19
When the whole world population has been vaccinated against certain contagious and malicious pathogenic agent, it creates a herd immunity to those people who are unable to be directly protected by vaccination. Herd immunity is defined as resistance to the spread of contagious disease (indirect protection) within a population which results from a sufficiently high proportion of individuals who are immune to the disease. However, herd immunity without coming from vaccination is not a preventative measure. For instance, COVID-19 basic reproduction rate (R0) is approximately 3.28, which means that in a susceptible population, each infected COVID-19 person will pass the disease on to 3 – 4 people17. Roughly, once there is four or more infections have been introduced into susceptible population, there is over 50% chance that an outbreak will occur18. With R0 of 3.28, the proportion of people who needs to be infected is around 70% of the entire population which brings us to reason why herd immunity (without coming from vaccination) could never be considered as preventative measure. Plus, the impact of COVID-19 fatality rate is around 0.5%- 1% which means, if 70% of entire population gets infected, it means that between 0.35%-0.7% of entire population could possibly die, which is a catastrophic consequence.
In addition, there is no evidence that recovered patients with existing SARS-CoV-2 antibodies are protected from a second infection of COVID-1919. According to WHO, most studies reported that recovered patients have the antibodies against the virus but, some of these patients have a very low levels of neutralizing antibodies in their blood19. Thus, herd immunity during pandemic is unrealistic and take it as preventative strategy for COVID-19 is simply wrong. Herd immunity is able to achieve once the vaccine is developed and the availability of COVID-19 vaccine is the only solution to stop the pandemic from its tracks. A universal world acceptance for vaccination is able to eradicate COVID-19 since no vulnerable host is available.
Development of COVID-19 vaccine
A COVID-19 vaccine is a theoretical vaccine against SARS-CoV-2. Although no vaccine presently available but, a robust research effort is now on-going with multiple attempts of clinical trials in progress to develop such a vaccine. A vaccine works by educating the immune system to identify and fight against pathogens, either viruses or bacteria. Thus, a particular antigen from the pathogen must be presented into the host body to activate an immune response. By inoculating the antigens into the body, the immune system able to carefully learn to identify them as hostile intruders and thus, produce antibodies against them and memorise them for the future threaten. If the same pathogen returns in the host body, the immune system will recognise the antigens spontaneously and aggressively attack them before they can trigger and spread the disease inside the host.
Presently, the Coalition for Epidemic Preparedness Innovations (CEPI) is working together with international health authorities and vaccine developers to support the COVID-19 vaccines development. As of 8th April 2020, there are 115 vaccine candidates have been included into global COVID-19 vaccine R&D landscape20. Apart from this, 78 confirmed active projects and 73 on preclinical stages. In April, CEPI researchers have reported 10 different vaccine platforms under R&D during early 2020 to develop an effective COVID-19 vaccine20. However, the main platforms which progressed into clinical studies involving DNA and RNA vaccines, non-replicating viral vector vaccines and also recombinant protein vaccine. However, according to CEPI, DNA or mRNA vaccines provide promising results due to its strong immune responses, can be rapidly assessed, possess long-term stability and potential for a large-scale production capacity.
There are five vaccine candidates which recently progress into clinical development including mRNA-1273 from Moderna, United States (Phase 1: NCT04283461), Ad5-nCoV from CanSino Biologicals, China (Phase 1: NCT04313127), INO-4800 from Inovio Pharmaceuticals, United States (Phase 1: NCT04336410), LV-SMENP-DC (Phase 1: NCT04276896) and pathogen-specific aAPC (Phase 1: NCT04299724) from Shenzhen Geno-Immune Medical Institute, China20.
The mRNA-1273 vaccine candidate from Moderna Inc. is a novel lipid nanoparticle-encapsulated mRNA-based vaccine which encodes for a full-length, prefusion stabilised spike protein of COVID-1921. Moderna Inc. is a Cambridge, Massachusetts-based biotechnology company which focus on drug discovery and development based on mRNA22. The mRNA-1273 vaccine contains of an mRNA drug substance which is manufactured into lipid nanoparticle composed of the proprietary ionisable lipid and three other commercially available lipids21. They have started Phase I clinical trial of mRNA-1273 vaccine in 45 participants of healthy adult volunteers in March, 2020. The participants received intramuscular injection of mRNA-1273 on Day 1 and Day 29 in the deltoid muscle concurrently, with a follow-up visit through 12 months of post second vaccination. The main objective of the trial is to measure the safety and reactogenicity of a 2-dose vaccination schedule (28 days apart) of mRNA-1273 in healthy adults21. The second objective is to assess the immunogenicity to COVID-19 spike protein following a 2-dose vaccination schedule by measuring immunoglobulin G by enzyme-linked immunosorbent assay (ELISA)21.
The second vaccine candidate, Ad5-nCoV is developed by CanSino Biologics Inc, China. This biopharmaceutical company develops and manufactures biological vaccine products such as quadrivalence meningococcal conjugate, pneumococcal polysaccharide and adenovirus vector-based tuberculosis vaccines for human use23. This vaccine candidate is genetically engineered with replication-defective adenovirus type 5 vector which express the COVID-19 spike protein. The Ad5-nCoV vaccine also the first candidate which enters Phase II clinical trial on 15 April 202024. The trial is a single-centre, open-label, dose-escalating which involves 108 participants of healthy adult volunteers in March, 2020. The participants of 3 different groups (low-dose, middle-dose and high-dose groups) receive intramuscular injection of Ad5-nCoV vaccine or placebo on Day 1 in deltoid muscle. The primary outcome is to evaluate the safety, reactogenicity and immunogenicity of Ad5-nCoV vaccine in healthy adults24. The secondary outcome is to measure the humoral immunity and cellular immunity in terms of dose-response relationship and time-dose-response relationship in the subjects24.
Third vaccine candidate is a DNA-based vaccine from Inovio Pharmaceuticals, United States. Inovio Pharmaceuticals is a biopharmaceutical company which focuses on the discovery, development and commercialisation of synthetic DNA products for treating cancers and infectious diseases25. The INO-4800 vaccine is genetically engineered from DNA plasmid which encodes the spike protein of COVID-19 that is delivered by a particular device via electroporation method. The vaccine carries optimised DNA plasmids directly into host cells via intramuscular or intradermal using CELLECTRA® 2000 device. The device utilises a brief electrical pulse to expose small pores in the host cell reversible to allow the DNA plasmids to enter26. Once within the host cell, the DNA plasmids are utilised by cell’s own machinery to construct specific coded antigens, which then stimulate an immune response. The trial is an open-label, dose-escalating which involves 40 participants of healthy volunteered participants in April, 2020. Two experimental groups received two different doses of INO-4800 vaccine followed by electroporation using CELLECTRA® 2000 device on Day 0 and Week 427. The primary outcome is to measure the safety, tolerability and immunological profile of INO-4800 in healthy adult volunteers.
Lentiviral synthetic mini-gene vaccine targeting dendritic cells (LV-SMENP-DC) from Shenzhen Geno-Immune Medical Institute, China is the fourth vaccine candidate listed for Phase I clinical trial for COVID-19. Shenzhen Geno-Immune Medical Institute is a government institute from Shenzhen Province that offers contracted research and technical assistances for individually cell-based immunotherapy28. The LV-SMENP-DC vaccine is a dendritic cells modified with lentiviral vector system (NHP/ TYF) expressing the selected viral synthetic mini-gene protein that is administered into host body with antigen-specific cytotoxic T cells (CTLs)20. A hundred of volunteered participants are involved in the Phase I clinical trial which estimated to complete on December, 2024. The primary objective is to evaluate the safety of injection and infusion of LV-SMENP-DC and antigen-specific T cell vaccines on healthy adult volunteers and COVID-19 patients29. Their secondary objective is to measure the anti-COVID-19 efficacy of the LV-SMENP-DC and antigen-specific CTL vaccines29.
The last current vaccine candidate listed for Phase I clinical trial against COVID-19 is pathogen-specific aAPC also from Shenzhen Geno-Immune Medical Institute, China20. This vaccine uses the similar concept as LV-SMENP-DC vaccine, only they modified the artificial antigen presenting cells (aAPCs) to activate T cells30. A hundred volunteered participants also recruited into the study which estimated to end on July 31, 2023 for primary outcome. They receive three injections of each pathogen-specific aAPC vaccine via subcutaneous injections at Day 0, Day 14 and Day 28. Later, they are being followed-up with peripheral blood tests at Day 0, Day 14, Day 21, Day 28 and Day 60 until the end of the test. The primary outcome measures are the frequency of vaccine events such as fever, rash and abnormal heart function, frequency of serious vaccine events and proportion of subjects with positive T cell response30. Their secondary outcomes are 28-day mortality (number of deaths during study follow-up), duration of mechanical ventilation if applicable, proportion of patients with normalized inflammation factors, clinical improvements and Lower Murray lung injury score if applicable30.
These vaccine candidates on trials provide a seed of hope to humanity for a total eradication of COVID-19. Though its still a long way to finally have the vaccine but this hope keeps most of us to continue relentlessly fighting the virus for the sake of human mankind.
Malaysia landscape on vaccine development
In the current outbreak of SARS-CoV-2, Malaysia could be approximately in the middle compared to the other countries in the pandemic curve4. According to a report released by the WHO on 19 April 2020, the total number of confirmed cases is 5,305 whereas 88 deaths is the total number of deaths so far3. In a study to generate forecasts of COVID-19 cases in Malaysia, three statistical methods have been employed based on Malaysia Ministry of Health data until 1st April 202031. The three estimations were as follow: the peak will be on 19 April 2020 with approximately 5,637 confirmed cases; 2) the peak will be between 20 and 31 May 2020 with approximately 630,000 to 800,000 confirmed cases; 3) the peak will be on 17 May 2020 with approximately 22,421 confirmed cases.
Among several countries involved in the global “Solidarity Trial”, Malaysia contributes to test the safety and effectiveness of four treatment protocols using different combinations of Remdesivir, Lopinavir/ Ritonavir, Interferon beta, Chloroquine and Hydroxychloroquine32. These unmatched efforts are coordinated by the WHO and aim to set reliable data for using these protocols. Furthermore, thanks to the similarity between human coronavirus and avian coronavirus, Infectious Bronchitis Virus (IBV), Malaysia has joined the global race to develop vaccines for Covid-19. In collaboration with University of Malaya Tropical Infectious Diseases Research and Education Centre (TIDREC) and Malaysian Vaccines and Pharmaceutical Sdn Bhd (MVP), Institute for Medical Research Malaysia (IMR) has started testing existing IBV vaccines against SARS-CoV-233.
Conclusion
In summary, as COVID-19 causes a serious public health concerns worldwide, the world is urgently in need for new vaccines. Nevertheless, the major challenge remains. Across the years, the world experienced new major coronavirus epidemic every decade in twenty-first century-SARS in the 2000s, MERS in the 2010s and now COVID-19 in 2020. Therefore, an international security urgency is to progress and supply coronavirus vaccines, and to recognise global funding means to support their development, production and storage. In fact, this new pandemic should work as an encouragement to call upon the global research community to not only respond but also prepare for the subsequent coronavirus attack. A pan-coronavirus vaccine is urgently required and seems technically achievable if adequate resources are made available within time.
References:
- Zhu N, Zhang D, Wang W, Li X, Yang B, Song J. A Novel Coronavirus from Patients with Pneumonia in China, 2019. New England Journal of Medicine 2020;382(8):727-33.
- Event background COVID-19 [Internet] European Centre for Disease Prevention and Control; 2020 [cited 2020 April 20]. Available from: https://www.ecdc.europa.eu/en/novel-coronavirus/event-background-2019.
- Situation Report – 90 [Internet]. World Health Organisation; 2020 [cited 2020 April 20]. Available from: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200419-sitrep-90-covid-19.pdf?sfvrsn=551d47fd_4.
- 4. Roser M, Ritchie H, Ortiz-Ospina E, Hasell J. Coronavirus Disease (COVID-19) – Statistics and Research [Internet] Our World in Data; 2020 [cited 2020 April 18]. Available from: https://ourworldindata.org/coronavirus.
- Wu D, Wu T, Liu Q, Yang Z. The SARS-CoV-2 outbreak: what we know. Int J Infect Dis. 2020.
- Yang X, Yu Y, Xu J, Shu H, Xia Ja, Liu H. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. The Lancet Respiratory Medicine. 2020.
- Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. The Lancet 2020;395(10223):507-13.
- Linton NM, Kobayashi T, Yang Y, Hayashi K, Akhmetzhanov AR, Jung SM. Incubation Period and Other Epidemiological Characteristics of 2019 Novel Coronavirus Infections with Right Truncation: A Statistical Analysis of Publicly Available Case Data. J Clin Med 2020;9(2):2077-0383.
- Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020:e201585.
- Hu Z, Song C, Xu C, Jin G, Chen Y, Xu X. Clinical characteristics of 24 asymptomatic infections with COVID-19 screened among close contacts in Nanjing, China. Science China Life Sciences. 2020.
- Czochor J, Turchick A. Introduction. Vaccines. Yale J Biol Med 2014;87(4):401-2.
- Riedel S. Edward Jenner and the History of Smallpox and Vaccination. Baylor University Medical Center Proceedings 2005;18(1):21-5.
- Clem AS. Fundamentals of vaccine immunology. J Glob Infect Dis 2011;3(1):73-8.
- Cohen P, Scadron SJ. The placental transmission of protective antibodies against whopping cough: By inoculation of the pregnant mother. Journal of the American Medical Association 1943;121(9):656-62.
- Pulendran B, Ahmed R. Translating Innate Immunity into Immunological Memory: Implications for Vaccine Development. Cell 2006;124(4):849-63.
- Tahamtan A, Charostad J, Hoseini Shokouh SJ, Barati M. An Overview of History, Evolution, and Manufacturing of Various Generations of Vaccines. J Arch Mil Med 2017;5(3):e12315.
- Liu Y, Gayle AA, Wilder-Smith A, Rocklöv J. The reproductive number of COVID-19 is higher compared to SARS coronavirus. Journal of Travel Medicine 2020;27(2).
- Kucharski AJ, Russell TW, Diamond C, Liu Y, Edmunds J, Funk S. Early dynamics of transmission and control of COVID-19: a mathematical modelling study. The Lancet Infectious Diseases 2020;20(5):553-8.
- World Health Organization W. “Immunity passports” in the context of COVID-19. World Health Organization; 2020 April 20; [Available from: https://www.who.int/news-room/commentaries/detail/immunity-passports-in-the-context-of-covid-19]. English.
- Thanh TL, Andreadakis Z, Kumar A, Gómez Román R, Tollefsen S, Saville M. The COVID-19 vaccine development landscape. Nature Reviews Drug Discovery. 2020.
- National Institute of Allergy and Infectious Diseases N. Safety and Immunogenicity Study of 2019-nCoV Vaccine (mRNA-1273) for Prophylaxis SARS CoV-2 Infection (COVID-19) [Internet]. ClinicalTrials.gov; 2020 [cited 2020 April 20]. Available from: https://clinicaltrials.gov/show/NCT04283461.
- Moderna I. mRNA: A new approach to medicine. Moderna Inc; 2020 April 20; [Available from: https://www.modernatx.com/modernas-mrna-technology]. English.
- CanSino Biologics I. Corporate profile of CanSino Biologics Inc [Internet]. CanSino Biologics Inc; 2017 [cited 2020 April 20]. Available from: http://www.cansinotech.com/homes/onepage/index/39.html.
- CanSino Biologics I. Phase I Clinical Trial of a COVID-19 Vaccine in 18-60 Healthy Adults [Internet]. ClinicalTrials.gov; 2020 [cited 2020 April 20]. Available from: https://clinicaltrials.gov/show/NCT04313127.
- Inovio Pharmaceuticals I. About leadership in Inovio [Internet]. Inovio Pharmaceuticals; 2019 [cited 2020 April 20]. Available from: https://www.inovio.com/.
- INOVIO initiates Phase I clinical trial of its COVID-19 vaccine and plans first dose today [press release]. Inovio Pharmaceuticals Inc. 2020 April 20; [Available from: http://ir.inovio.com/news-and-media/news/press-release-details/2020/INOVIO-Initiates-Phase-1-Clinical-Trial-Of-Its-COVID-19-Vaccine-and-Plans-First-Dose-Today/default.aspx]. English.
- Inovio Pharmaceuticals I. Safety, Tolerability and Immunogenicity of INO-4800 for COVID-19 in Healthy Volunteers [Internet]. ClinicalTrials.gov; 2020 [cited 2020 April 20]. Available from: https://clinicaltrials.gov/show/NCT04336410.
- Shenzen Geno-Immune Medical Institute S. About Shenzen Geno-Immune Medical Institute [Internet]. Shenzen Geno-Immune Medical Institute; 2016 [cited 2020 April 20]. Available from: http://www.szgimi.org/en/about.php.
- Shenzhen Geno-Immune Medical Institute S. Immunity and Safety of Covid-19 Synthetic Minigene Vaccine [Internet]. ClinicalTrials.gov; 2020 [cited 2020 April 20]. Available from: https://clinicaltrials.gov/show/NCT04276896.
- Shenzhen Geno-Immune Medical Institute S. Safety and Immunity of Covid-19 aAPC Vaccine [Internet]. ClinicalTrials.gov; 2020 [cited 2020 April 20]. Available from: https://clinicaltrials.gov/show/NCT04299724.
- Salim N, Chan WH, Mansor S, Bazin NEN, Amaran S, Faudzi AAM. COVID-19 epidemic in Malaysia: Impact of lock-down on infection dynamics. medRxiv. 2020.
- Couillard C, Pin GP. Malaysia starts global “Solidarity Trial” - a research effort to test possible treatments for COVID-19. World Health Organization; 2020 April 27; [Available from: https://www.who.int/malaysia/news/detail/05-04-2020-malaysia-starts-global-solidarity-trial---a-research-effort-to-test-possible-treatments-for-covid-19]. English.
- IMR begins testing to develop vaccines for Covid-19. New Straits Times. 2020 April 27; [Available from: https://www.msn.com/en-my/news/national/imr-begins-testing-to-develop-vaccines-for-covid-19/ar-BB11Gckg]. English.
